-
The Workplace Has Failed to Adapt to Mothers’ Needs — and It’s Taking a Toll
›
“I don’t wanna work anymore,” the comedian Ali Wong exclaimed in front of her audience on her recent Netflix stand-up show — she was heavily pregnant at the time. “Well, I don’t wanna lean in, OK? I wanna lie down,” she added, referring to Lean In, the iconic career advice book for women. The crowd roared with laughter.
-
Eliane Razafimandimby: Improving the Quality of Maternal and Child Care
› “Even in a weak system without a quality improvement structure, it is possible to support district managers and facility providers to measure and improve quality care,” said Eliane Razafimandimby, Chief of Party of USAID’s flagship Maternal and Child Survival Program (MCSP) in Madagascar, at a recent Wilson Center event on improving the quality of reproductive, maternal, newborn, and child healthcare (RMNCH).
“Even in a weak system without a quality improvement structure, it is possible to support district managers and facility providers to measure and improve quality care,” said Eliane Razafimandimby, Chief of Party of USAID’s flagship Maternal and Child Survival Program (MCSP) in Madagascar, at a recent Wilson Center event on improving the quality of reproductive, maternal, newborn, and child healthcare (RMNCH). -
How to Value Unpaid Care Work: The $10 Trillion Question
›
In Judy Brady’s iconic essay, “I Want a Wife,” the feminist activist enumerates the dozens of practical and emotional tasks wives perform as a matter of duty. At the end, she asks: “My God, who wouldn’t want a wife?”
-
Everybody Counts: Saving the World One Condom at a Time
› Can we save the world one condom (or birth control pill) at a time? The third episode of Everybody Counts, hosted by Jennifer D. Sciubba, a professor of political demography at Rhodes College, makes the case that family planning is the foundation of peace and security by highlighting the links between population growth and political instability.
Can we save the world one condom (or birth control pill) at a time? The third episode of Everybody Counts, hosted by Jennifer D. Sciubba, a professor of political demography at Rhodes College, makes the case that family planning is the foundation of peace and security by highlighting the links between population growth and political instability. -
Saving Lives: Focusing on Outcomes to Improve Maternal and Newborn Healthcare Quality
›
Poor quality care is now a bigger barrier to reducing mortality than insufficient access to healthcare, said Dr. Margaret Kruk, Chair of The Lancet Global Health Commission on High Quality Health Systems in the Sustainable Development Goal Era. She spoke at a recent Wilson Center event on strategies to improve and sustain high-quality reproductive, maternal, and newborn care at scale. “We estimate that 8.6 million lives are lost every year due to lack of access to high quality care, and of that 8.6 million, five million lives are lost by people who have already reached out to the health system.”
-
Ageing Populations Could Create a Care Crisis—Or Millions of Jobs
›
The silver tsunami is approaching: Many countries, not all of them rich, are facing the challenges of an ageing population thanks to growing life expectancies and shrinking birth rates.
-
Mothers on the Front Lines: Armed Conflict, Aid Distribution, and Maternal and Child Health
›
While most people killed in wars are male, several studies have found that “mortality among women in some high-intensity conflicts was as severe as male mortality,” said Henrik Urdal, the Director of the Peace Research Institute Oslo (PRIO), at a recent Wilson Center event on the links between maternal and child health, aid, and armed conflict. “Maternal health is a very natural place to start” when researching excess mortality and indirect deaths among women impacted by war, said Urdal.
-
Too Little Too Late: Violence Disrupts Maternal Health Care in Conflict Settings
› “One of the first victims of war is the health care system itself,” said Marco Baldan, the chief war surgeon for the International Committee of the Red Cross. Violence directed at health facilities and workers is common in conflict, despite international laws protecting medical personnel, facilities, and transport vehicles during war.
“One of the first victims of war is the health care system itself,” said Marco Baldan, the chief war surgeon for the International Committee of the Red Cross. Violence directed at health facilities and workers is common in conflict, despite international laws protecting medical personnel, facilities, and transport vehicles during war.
Showing posts from category Dot-Mom.


 “Even in a weak system without a quality improvement structure, it is possible to support district managers and facility providers to measure and improve quality care,” said
“Even in a weak system without a quality improvement structure, it is possible to support district managers and facility providers to measure and improve quality care,” said 
 Can we save the world one condom (or birth control pill) at a time? The third episode of
Can we save the world one condom (or birth control pill) at a time? The third episode of 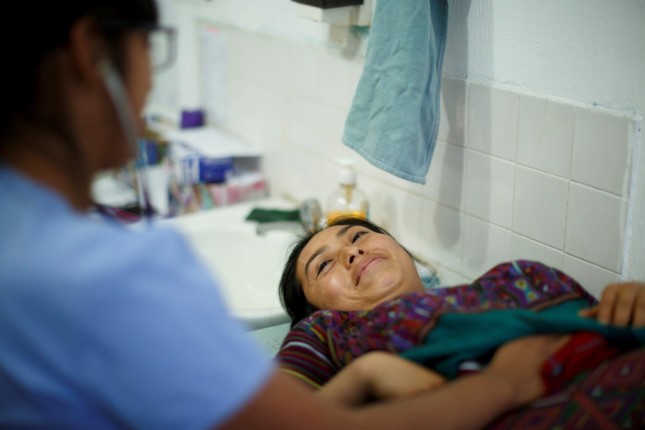


 “One of the first victims of war is the health care system itself,”
“One of the first victims of war is the health care system itself,” 

