-
Patricia Da Silva: ‘The Time is Now’ to Accelerate Progress for Sexual and Reproductive Health and Rights
› “Almost everyone of reproductive age—about 4.3 billion people—will not have access to at least one essential or reproductive health intervention over the course of their lives,” said Patricia Da Silva, Associate Director, International Planned Parenthood Federation United Nations Liaison Office. She spoke at a recent Wilson Center event showcasing recommendations from the Guttmacher-Lancet Commission report, “Accelerate progress–sexual and reproductive health and rights for all,” on how to advance sexual and reproductive health from a human rights perspective.
“Almost everyone of reproductive age—about 4.3 billion people—will not have access to at least one essential or reproductive health intervention over the course of their lives,” said Patricia Da Silva, Associate Director, International Planned Parenthood Federation United Nations Liaison Office. She spoke at a recent Wilson Center event showcasing recommendations from the Guttmacher-Lancet Commission report, “Accelerate progress–sexual and reproductive health and rights for all,” on how to advance sexual and reproductive health from a human rights perspective. -
Caring for Others is Making Women Ill. What Can Government Do?
›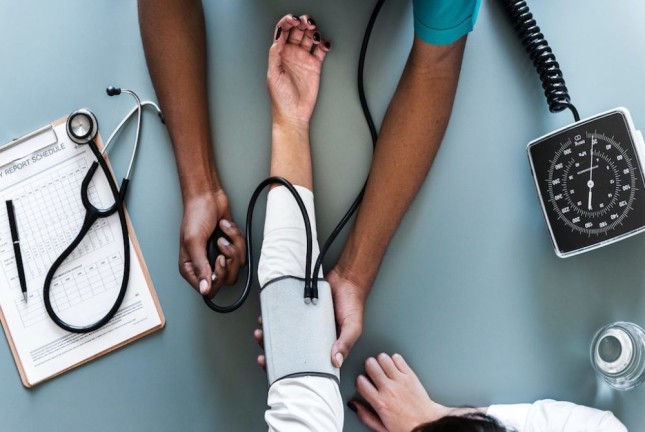
Whether it’s thanks to shouldering the majority of unpaid care work, or facing poor conditions in their roles as paid carers, women laboring in the care economy face serious threats to their health.
-
More Countries Want to Invest in Caring. Here’s How They Should Do It
›
At long last, my husband and I are empty-nesters. We have always worked in high-pressure jobs, and while the children were young, I put in plenty of non-work hours to care for them and for the household. My husband was unfailingly helpful, but now that our children are grown, I’m ready to renegotiate our “to do” list.
-
Innovative Approaches Empower Adolescent Girls to Live HIV-free Lives
›
“Everyone in the community knew that I was the next [to get pregnant], but I was so determined that until I achieve my dream of becoming an accountant, I will not drop out of school, and I will not get pregnant,” said Rebecca Acio, a 19-year-old Ambassador for the Strengthening School-Community Accountability for Girls’ Education (SAGE) DREAMS Project, Uganda. She spoke at a recent Wilson Center event on emerging lessons from the DREAMS Innovation Challenge. As a peer educator at her school in Lira, Uganda, and a temporary dropout herself, Acio “knew what it cost to be a dropout” and worked to identify other at-risk girls to encourage them to stay in school.
-
How a Healthcare Company is Helping Tackle Unpaid Carers’ Health Problems
›
As populations age, countries around the globe are beginning to focus attention on unpaid caregivers. Such people typically spend hours each day bathing, feeding, and helping an elderly or disabled relative. Often, they undermine their own health and career to take care of a loved one.
-
Senator Nikoli Edwards: Adolescent Health and Investing in a Generation
›In January 2017, President Anthony Carmona swore in Nikoli Edwards, age 25, as the youngest temporary senator in Trinidad and Tobago’s history. “I have been very much involved in piecing together the puzzle when it comes to how we develop the holistic young person in Trinidad and Tobago,” said Senator Nikoli Edwards in a Wilson Center interview with Roger-Mark De Souza, a Wilson Center Global Fellow, on Edwards’s personal journey into youth advocacy and the importance of engaging young people in decision-making.
-
Cultivating Meaningful Youth Engagement in Sexual and Reproductive Health Programming
› “We need to mainstream young people into the decision-making process,” said Senator Nikoli Edwards, age 25, of Trinidad and Tobago at a recent Wilson Center event on engaging youth to protect their sexual and reproductive health and rights. “Where it’s not a matter of, ‘let’s bring a young person into the room as an afterthought,’ but it should be written that a young person has to be a part of the discussion or has to be contributing in a significant way.”
“We need to mainstream young people into the decision-making process,” said Senator Nikoli Edwards, age 25, of Trinidad and Tobago at a recent Wilson Center event on engaging youth to protect their sexual and reproductive health and rights. “Where it’s not a matter of, ‘let’s bring a young person into the room as an afterthought,’ but it should be written that a young person has to be a part of the discussion or has to be contributing in a significant way.” -
“Norway’s “Daddy Quota” Means 90 Percent of Fathers Take Parental Leave”
›
Visitors to Norway often remark on the number of men pushing prams around its streets. This summer, those pram-pushing days are growing longer, and not just because of the endless sun. Fathers of children born on or after July 1 will get 15 weeks non-transferable parental leave, rather than the already-generous 10 previously available.
Showing posts from category Dot-Mom.


 “Almost everyone of reproductive age—about 4.3 billion people—will not have access to at least one essential or reproductive health intervention over the course of their lives,” said Patricia Da Silva, Associate Director, International Planned Parenthood Federation United Nations Liaison Office. She spoke at a
“Almost everyone of reproductive age—about 4.3 billion people—will not have access to at least one essential or reproductive health intervention over the course of their lives,” said Patricia Da Silva, Associate Director, International Planned Parenthood Federation United Nations Liaison Office. She spoke at a 

 “We need to mainstream young people into the decision-making process,” said Senator Nikoli Edwards, age 25, of Trinidad and Tobago at a
“We need to mainstream young people into the decision-making process,” said Senator Nikoli Edwards, age 25, of Trinidad and Tobago at a 


