Showing posts from category Kenya.
-
Championing Women’s Rights and Population Issues in Kenya With the ‘Reject’
› “We find that politicians play around with [population] numbers when it comes to the common man and the common woman,” says Jane Godia in this short video interview. Godia writes for Reject, an African Woman and Child Feature Service biweekly news publication that won a Global Media Award from the Population Institute for its issue on family planning and politics in Kenya.
“We find that politicians play around with [population] numbers when it comes to the common man and the common woman,” says Jane Godia in this short video interview. Godia writes for Reject, an African Woman and Child Feature Service biweekly news publication that won a Global Media Award from the Population Institute for its issue on family planning and politics in Kenya.
Godia says that politicians “use these numbers for their gain, they tell women not to use family planning because they want more children so that…they can have more voters, but nobody thinks about if this woman will be able to feed these children, if this family will be able to have their next meal, or even accommodation, or even land to till.”
The Reject’s name comes from the paper’s early practice of running stories – often about underserved groups, like women, children, and the poor – that had been rejected from mainstream publications. Population and environment issues have been highlighted since the first issue came out in September 2009, when “we were talking about families moving on to Mount Kenya…to look for pasture and water for their animals,” says Godia.
“When there’s no water and when there’s no food, people migrate,” she says. “And when people are migrating they’re moving with their animals, they’re moving with their families, and they end up going to places” that eventually become overcrowded and resource-stressed, sometimes introducing the same problems that led people to migrate in the first place. -
Delivering Solutions: Advancing Dialogue to Improve Maternal Health
›“Throughout the 2009-2011 Advancing Dialogue on Maternal Health lecture series, we always heard the same good news: we know how to save the lives of women and girls. But more political will is needed,” said Calyn Ostrowksi, program associate for the Wilson Center’s Global Health Initiative on December 15 for the launch of the series’ culminating report, Delivering Solutions: Advancing Dialogue To Improve Maternal Health.
Joining Ostrowski were co-author Margaret Greene, director of GreeneWorks; Luc de Bernis, senior advisor on maternal health at the UN Population Fund; Tim Thomas, interim director for the Maternal Health Task Force; and Chaacha Mwita, director of communications at the African Population and Health Research Center.
One of the few forums dedicated to maternal health, the series brought together senior-level policymakers, academic researchers, members of the media, and NGO workers from the United States and abroad. The series consisted of 21 separate events, with hundreds of experts sharing their experiences and thousands of participants and stakeholders providing their expertise. The final report captures, analyzes, and synthesizes the strategies and recommendations that emerged from the series.
Promoting Social Change
Unlike other health issues, said Green during her presentation on the findings of Delivering Solutions, the field of maternal health requires a holistic and multi-faceted approach; that is, an approach that looks not only at health systems, but also at underlying social factors. The report divides maternal health into three broad categories: social, economic, and cultural factors; health systems factors; and research/data demands.
Looking first at the social, cultural, and economic issues, Greene highlighted the need to improve nutrition and educational opportunities for young women in developing countries. Policymakers must be convinced that investing in women is not just good for women but good for families and children, she said. The participation of male partners and other male family members is also needed to increase access to maternal health services, such as family planning, and promote gender equality. The report pointed to a number of recommendations to promote male engagement:- Target interventions that educate men about danger signs and pregnancy complications.
- Address pressures that many young married men feel to prove their fertility.
- Inform men about sexual rights and how they relate to the health and wellbeing of their partners.
Health systems and medical resources play an equally pivotal role in reducing maternal mortality as social factors. The report highlights several key areas for strengthening the health system including the expansion of healthcare workers, health finance schemes, technology, and commodity distribution.
One key recommendation is to integrate reproductive health and maternal health supply chains. Four key medicines, oxytocin misoprostol, magnesium sulfate, and manual vacuum aspirators, target the three leading causes of maternal mortality (post-partum hemorrhage, obstructed labor, and unsafe abortion). Efforts to improve the distribution of these commodities should be more widely dispersed in developing countries and supported by community-based interventions. Women in urban slums, for example, face unique challenges that are not being adequately addressed.
Additionally, new technologies should be more creatively and effectively used, in particular the use of mobile phones in rural communities.
Many of the policy recommendations offered by the report, as Greene pointed out, are low-cost and highly effective. Yet three significant challenges remain for the field in general:- Six countries – Afghanistan, Democratic Republic of Congo, Ethiopia, India, Nigeria, and Pakistan – account for over half of the maternal deaths worldwide. The unique problems of each of these countries must be addressed and solved.
- Integration of maternal health with existing health services along with an over-reliance on community health workers can overburden weak infrastructure.
- Unnecessary cesarean births are on the rise as more women deliver in private sector facilities. These births cost 2 to 18 times as much as vaginal births and create unnecessary risks for mothers.
Chaacha Mwita of the African Population and Health Research Center (APHRC), located in Nairobi has seen firsthand the result of an overburdened and inadequate maternal health system in both his personal and professional life. Mwita endorsed the findings of the series report, emphasizing in particular the focus on transportation systems, male involvement, stakeholder dialogue, and education.
Mwita said that collaboration at all levels is the key to improving maternal health. Policymakers must communicate with researchers, who, in turn, must communicate with doctors, nurses, and hospital administrators in the field. The collaborative in-country dialogue series between the Wilson Center and APHRC, he believes, was a highly useful and easily replicable way of encouraging dialogue among relevant stakeholders in the field.
The Big Picture
”Our hope is that we’ve been able to seed discussions,” said Tim Thomas of the Maternal Health Task Force, one of the co-sponsors of the maternal health series. “We hope those seeds will take root and flourish.” Luc de Bernis, senior maternal health advisor of UNFPA, echoed Thomas’ sentiments, emphasizing the need for continued dialogue.
While maternal health has drawn increased international attention, creating political agreement among policymakers is a complex and often difficult process. There has been marked, though uneven, progress in improving maternal health across the globe, but more must be done. The Delivering Solutions report provides a state of the field assessment as well recommendations for existing, easy-to-implement solutions.
Event Resources: -
Migration and Environmental Change, Minority Land Rights and Livelihoods
›Migration and Global Environmental Change: Future Challenges and Opportunities, from the UK Government Office for Science’s Foresight Programme, looks at how environmental change, including climate change, land degradation, and the degradation of coastal and marine ecosystems, over the next 50 years will affect migration trends. The report emphasizes that migration is a complex and multi-causal phenomenon, which makes it difficult to differentiate environmental migrants as a distinct group. Nevertheless, research suggests that global environmental changes will affect the drivers of migration, particularly economic forces, such as rural wages and agricultural productivity.
Though Foresight finds that many will use migration as an adaptation strategy that improves resilience to environmental change, they also point out that some affected individuals may become “trapped” in vulnerable situations, lacking the financial capacity to respond to environmental changes, while others may be able to move but will inadvertently enter more exposed areas, particularly, at risk urban centers. For recommendations, they stress the importance of strategic, long-term urban planning, and recognition within adaptation and development policies that migration can be part of the solution.
A study, released on December 5 by Minority Rights Group International, finds that minority communities in Kenya, Uganda, and South Sudan face significant challenges around access to and control of critical natural resources. The report, Land, Livelihoods, and Identities: Inter-Community Conflicts in East Africa, shows how rapid population growth, climate change, and globalization are increasing competition for land, water, and forest and mineral resources in territories traditionally occupied by minority groups. These pressures can undermine livelihoods and trigger multiple and overlapping conflicts, especially where ownership has not been formalized in law. The study also notes that women are doubly vulnerable as their access to land and resources is frequently mediated through customary law, which depends on their communities retaining control over traditional territory. Although the report makes national-level legal and policy recommendations, the authors note that some of the most effective resource management and conflict resolution strategies adapt traditional cultural practices to the current circumstances of communities. -
Jake Naughton, Pulitzer Center for Crisis Reporting
Pulitzer Center Launches Collaborative Reporting Project on Reproductive Health
› The original version of this article, by Jake Naughton, appeared on the Pulitzer Center for Crisis Reporting blog.
The original version of this article, by Jake Naughton, appeared on the Pulitzer Center for Crisis Reporting blog.
The Pulitzer Center launched its collaborative reproductive health-reporting project at this year’s International Conference on Family Planning (ICFP) in Dakar, Senegal. The project brings together four journalists from Africa and four from the United States who will collaborate to enhance local and international reporting about reproductive health across the continent.
The African journalists are Mae Azango of Liberia, Estelle Ellis of South Africa, Sam Olukoya of Nigeria, and Ken Opala of Kenya. Their U.S. counterparts are Christian Science Monitor correspondent Jina Moore; New Yorker editorial staffer Alexis Okeowo; and the Pulitzer Center’s managing director Nathalie Applewhite and visual media coordinator Jake Naughton.
More than two thousand reproductive health professionals and hundreds of journalists from all over the world participated in the conference, which sought to shine a spotlight on the unmet need for family planning services worldwide, and to focus on integrating family planning into general health services.
Continue reading on the Pulitzer Center for Crisis Reporting blog.
Video Credit: “Meet the Journalists: Dakar,” courtesy of the Pulitzer Center. -
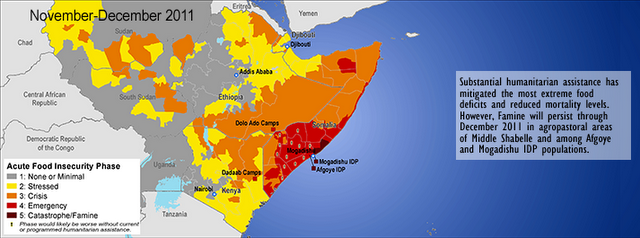
Famine and Food Insecurity in the Horn of Africa: A Man-Made Disaster?
›This year’s drought in the Horn of Africa has been the region’s worst in decades and has exploded into a humanitarian catastrophe affecting millions. In Somalia, where the drought is layered on top of two decades of conflict and an extremely weak state, the impact of the drought has been most damaging. Somalia is the only country in the region where the UN has declared famine zones. And, even though the UN recently upgraded three of Somalia’s six famine areas to “lesser emergencies,” four million Somalis – more than half the country’s population – remain in urgent need of food and general humanitarian aid.
The drought may have been what sparked the current crisis, but other, longer-term factors, like a sustained lack of agricultural development, extreme rural poverty, and changing weather patterns, not to mention Somalia’s lack of functioning government, set the stage.
A Long-Term Crisis in the Making
“Lack of rainfall over several seasons is the most immediate and most visible cause of the current humanitarian crisis in the Horn of Africa,” said Jim Hansen of the Consultative Group on International Agricultural Research (CGIAR) in a brief video produced this summer by the International Research Institute for Climate and Society at Columbia University (watch above). Much of the Horn’s population “depends on rain-fed agriculture and pastoralism for their livelihoods and sustenance,” said Hansen. Already “quite poor and…locked in poverty for quite a long time,” environmental and resource degradation, paired with rapid population growth, have compounded their vulnerability to extreme events, he said.
Throughout the region, resilience to crises like the current drought has been weakened by decades of poor agricultural planning, “driven more by shifts in ideology than any real evidence among some of the key international development organizations,” said Hansen. That poor planning has made communities more dependent on humanitarian aid when poor weather hits, which in turn forces aid groups to redirect resources away from longer-term development and towards short-term disaster relief instead, Hansen said.
While these problems exist across the Horn of Africa, Hansen points out that the crisis has been most damaging in Somalia, which he attributes to the country’s weak governance and to international aid groups’ limited ability to operate in the country.
“Northern Kenya, southern Ethiopia, and Somalia have similar severity of drought, but the humanitarian crisis is much more severe – the loss of livelihood and life is greater in Somalia largely because the government is weaker,” he said.
The Government’s Role
Owen Barder, a senior fellow at the Center for Global Development, draws a more direct line between governance and famine in the Horn. “In Somalia…there’s a complete breakdown of government, and the consequence is the famine that we’re seeing,” said Barder during a Center for Global Development podcast. The country has been without a functioning government since 1991, when civil war broke out. It has since become “the most food-insecure nation in the world” and, as described by Foreign Policy, “the international community’s longest-running failure.”
Barder raised two points about the government’s role in famine. One, that access to information – in this case an early warning system monitoring drought conditions – can minimize the humanitarian impact of any given natural disaster; and two, that a country’s government must be able to translate that information into action in order for it to actually make a difference.
Barder is not alone in emphasizing the state’s role as a driver of the famine. Edward Carr, a AAAS science fellow with USAID, wrote in July, when the UN first declared famine in Somalia, that attributing the famine solely to drought is “a horrible abdication of responsibility for the human causes of this tragedy.”
Charles Kenny, also a senior fellow at the Center for Global Development, went even further on Foreign Policy, arguing that famine, or “mass starvation as an intentional act of governance,” should be categorized as a crime and prosecutable at the International Criminal Court.
Al Shabab and the Months Ahead
As of late November, the United Nations estimated that tens of thousands had died in Somalia alone since drought began this spring. Though USAID’s Famine Early Warning Systems Network (FEWSNET) reports that famine has now subsided in three of the six southern regions it initially struck, a quarter of a million Somalis remain at risk of “imminent starvation,” according to the UN.
According to FEWSNET, famine should not reappear in the foreseeable future, assuming aid groups can maintain current distribution levels – a key caveat. Ten days after FEWSNET issued its analysis, however, Al Shabab, the Al Qaeda-linked militant organization that controls much of southern Somalia, banned 16 aid groups, including UNICEF and the World Health Organization, from operating in the areas under its control. UNICEF spokesman Jaya Murthy told the BBC that the move would put “about 160,000 severely malnourished children…at imminent risk of death.”
Fighting in southern Somalia between Al Shabab and Kenyan and Ethiopian forces is adding another layer to the country’s humanitarian crisis. The UN Office of the High Commissioner for Refugees reported that, as of late November, the fighting had become the primary driver of internal displacement, replacing drought and famine as the key drivers during the first three quarters of the year. The UNHCR estimated that, between the drought and the conflict, 1.46 million Somalis have been displaced.
Meanwhile, the rainy season is picking up, and although that’s good news for farmers and pastoralists, it also means that Somalis will be vulnerable to diseases like measles, typhoid, and cholera, which can spread quickly through overcrowded, under-supplied IDP camps. Somalis still living under Al Shabab’s control are prohibited from getting vaccinations, amplifying their vulnerability to disease in the coming months.
These latest developments offer strong evidence that policy decisions can exacerbate the human toll of natural disasters. From Barder’s perspective, that is reason for optimism. “We have the information, we have the capacity to prevent it from happening,” he said.
For more on Somalia’s underlying demographic issues, see Elizabeth Leahy Madsen’s post “In Somalia, Beyond the Immediate Crises, Demography Reveals a Long-Term Challenge.”
Sources: AlertNet, Associated Press, BBC, Famine Early Warning Systems Network, Foreign Policy, Huffington Post, The New York Times, UNHCR, UN News Centre, Voice of America.
Video Credit: “Jim Hansen on Food Security in East Africa,” courtesy of the International Research Institute for Climate and Society on vimeo; image credit: FEWSNET/USAID. -
New Population, Health, and Environment Program for Lake Victoria
›With some of Africa’s highest population densities, ethnic diversity, and biodiversity, the Great Lakes region is one of the most volatile intersections of human development and the environment. A new population, health, and environment (PHE) initiative from Pathfinder International, announced Monday at the International Conference on Family Planning in Senegal, aims to help address these issues by supporting sustainable resource management and women’s right to choose when and how often they have children.
Jointly funded by the David and Lucile Packard Foundation and the John D. and Catherine T. MacArthur Foundation, with additional support from USAID’s Office of Population and Reproductive Health, the project will focus on Ugandan and Kenyan sections of the Lake Victoria basin.
Lake Victoria is the second largest freshwater source in the world, a biodiversity hotspot, and an important regional waterway, but regional population growth among the highest in Africa and economic development have led to declining water quality, reduced fish stocks, and industrial pollution. The basin as a whole supports upwards of 35 million people.
“This new project is a welcome development for many reasons,” said ECSP Director Geoff Dabelko. “It brings the integrated PHE approach to one of the world’s greatest lakes, it enables respected health NGO Pathfinder to pursue PHE efforts, and marks the return of a leading private donor, the MacArthur Foundation, to a group of foundations willing to support this innovative approach.”
Sono Aibe, senior advisor for strategic initiatives at Pathfinder emphasized the integrated challenges facing the region. “In these remote, resource dependent areas of the world, the interconnectedness between the health of people and the health of the environment is undeniable,” she said in a press release. “When women are empowered to participate in the sustainable management of natural resources alongside men and youth, as well as have access to sexual and reproductive health care services, their lives will improve and so will the condition of the ecosystems that they depend on.”
The project’s objective, according to Pathfinder, is to reduce threats to biodiversity, conservation, and ecosystem degradation by increasing access to family planning and sexual/reproductive health services. The project plans to develop scalable approaches that can be adopted by communities, local governments, and national governments. Technical support is to be provided by the BALANCED Project, ExpandNet, and the Population Reference Bureau.
“Lessons learned from this new project will help us better develop and design projects for vulnerable communities in fragile ecosystems, while simultaneously advocating for increased government support for integrated programs throughout the Lake Victoria Basin,” said Lucy Shillingi, Pathfinder’s country representative for Uganda.
The Lake Victoria effort will build upon the experiences of other integrated PHE efforts in the region, such as Rwanda’s SPREAD Project, Uganda’s Conservation Through Public Health, and Tanzania’s TACARE and Coastal Management Partnership.
Sources: Lake Victoria Basin Commission, Pathfinder International, UNEP. -
Healthy People, Healthy Ecosystems: Results From a Public-Private Partnership
›“A lot of people probably don’t think that an organization with a name like ‘World Wildlife Fund’ would have a program on population, health, and the environment,” said WWF’s Tom Dillon at the Wilson Center, but actually it is very natural. “Most of the people we work with are in rural areas, and they depend on their natural resources for their own livelihoods and for their own well-being. Of course, if you are in that situation, in order to be a steward of the environment, you’ve got to have the basics. You have got to have your own health.”
Dillon was joined by staff from WWF, as well as Scott Radloff, director of USAID’s Office of Population and Reproductive Health, and Conrad Person, director of corporate contributions at Johnson & Johnson, to talk about the results of a three-year partnership between USAID, WWF, and Johnson & Johnson. The joint effort, a formal Global Development Alliance, provided health and family planning services, clean water, and sanitation to communities in three of WWF’s priority conservation landscapes: The Salonga National Park in the Democratic Republic of Congo (DRC), the Lamu Archipelago in Kenya, and the Terai Arch Landscape in Nepal.
By creating an innovative public-private partnership that linked health objectives, particularly related to family planning and maternal and child health, to environmental and conservation activities, “this alliance was ahead of its time,” said Radloff.
Human Health Linked to Environmental Health
The project had four objectives, said Terri Lukas, WWF’s population, health, and environment (PHE) program manager: improve family health; reduce barriers to family planning and reproductive health services; improve community management of natural resources and habitat conservation; and document and promote successful approaches.
“Human health cannot be separated from environmental health anywhere,” Lukas said, “but most especially when we are working with very poor people who live very close to nature.”
Projects Provide Integrated Services
The Salonga National Park in the DRC is home to many endangered species, including the bonobo, one of the four great apes. Local communities are very isolated, and lack access to safe drinking water and sustainable livelihoods, as well as basic health and family planning services, according to Lukas. The PHE project was able to train 135 voluntary community health workers in family planning and maternal and child health care, including 55 women. One year after the training, health workers were distributing contraception to more than 300 new users per month, Lukas said.
The alliance has also integrated health and family planning services into conservation programs in Kenya’s Kiunga Marine National Reserve, in part, “to demonstrate to the people that we care about them as well as the environment, and also to show them the synergies that exist between the health issue and the environment issue,” said WWF Program Coordinator Bahati Mburah. The region has been suffering through a year-and-a-half-long drought, and has one of the highest population growth rates in east Africa, placing considerable pressure on natural resources.
“We talk to [the fisher folk] about health and family planning, and how they are related to the management of fisheries,” said Mburah. With improved transportation and mobile outreach services provided by the project, 97 percent of women are now able to access family planning services within two hours of their home, she said.
The third site is in the Terai region along the southern border of Nepal. In this lowland region, the alliance is attempting to safeguard and restore forest areas in order to allow wildlife to move and breed more freely, while at the same time improving the health and economic prospects of the people. By linking these goals, support for conservation efforts increased from 59 percent to 94 percent of households, with 85 percent attributing positive attitude changes to increased access to health services and safe drinking water, according to Bhaskar Bhattarai, project coordinator for WWF-Nepal.
Documenting and Promoting Successful Approaches
Cara Honzak, WWF’s senior technical advisor on population, health, and environment, said the global objective of the alliance was to document and promote successful PHE approaches. Comprehensive baseline and endline surveys provided critical evidence that integrated PHE programming increases family planning use in remote areas, improves conservation buy-in within communities, and leads to increased participation of women in community leadership and decision-making.
“We have played a key role in producing some of the evidence that has been used throughout Washington [D.C.], especially to provide information to government bodies that are making decisions about bringing more money into family planning, health, and particularly in the environmental sector,” said Honzak.
“After two decades in the field, and working in this area, I wasn’t expecting many surprises. I couldn’t have been more wrong,” Lukas said. “These three years have changed almost everything about the way I now view health development…I have long called myself a conservationist, but now I say to my international health colleagues: we are all conservationists, and if we aren’t, we should be.”
Event Resources- Bhaskar Bhattarai presentation
- Cara Honzak presentation
- Terri Lukas presentation
- Bahati Mburah presentation
- Photo gallery
- Video
-
Emily Puckart, MHTF blog
Maternal Health in Kenya: New Research Unnecessary, Time to Address Existing Gaps
›The original version of this article, by Emily Puckart, appeared on the Maternal Health Task Force blog.
During the recent Wilson Center/African Population and Health Research Center meeting in Nairobi on improving health systems through a maternal health framework, participants focused on knowledge gaps in the Kenyan health system that can negatively affect maternal healthcare. This focus on gaps sparked discussion around research needed (or not needed) in the maternal health field, supply gaps, and gaps between addressing technical, medical issues of maternal health (like preeclampsia or postpartum hemorrhage), and larger society-wide gaps like gender equity. The gaps highlighted by participants at the Nairobi dialogue included:- Gaps in knowledge: During the dialogue, members of the Kenyan maternal health community discussed the possibility of strengthening community health workers as an information delivery platform. Participants wondered about the possibility of using community health workers to distribute information both downward to the end user (patients), and then again to gather information from end users and distribute it upwards through the system to reflect the opinions of the direct users of the healthcare system.
- Supply gaps: Participants argued that while there is a large body of information in terms of maternal health supplies at the national level in Kenya, there is not as much data on supplies at the actual health facility level, where it is much needed and would be very helpful to successfully treat patients.
- Gaps in healthcare delivery: There is a strong need to address inequality in the distribution of health services as there are unequal services in rural and urban areas. Within those broad areas there may be further inequalities, as even in urban areas, slum areas or neighborhoods on the edges of cities may have less access to quality healthcare than populations that live in wealthier areas of the city or closer to the city center. Further there are broader questions of gender and access to care. Where women are not able to control household finances, they may be unable to access and pay for lifesaving care. Participants framed the question in a rights framework, “Do we value the lives of women less than men?”
- Health workforce gaps: There is a mismatch between the supply of health workers and the absorption of those trained health workers in Kenya. Many of them are not incentivized professionally or financially to stay in the system where they are trained. These health workers may leave for other countries or prefer to stay in urban areas depriving rural areas of a surplus of trained health workers.
- Gaps between words and actions: Several of the small working groups pointed to accountability as a serious issue, as there are gaps between the words of politicians on health issues and actual actions. The gap between the government promised funding for health and the actual lower amount of spending was consistently highlighted during the Nairobi dialogue as a serious gap in holding governments accountable for their promises.
The lively conversation provoked by a broad discussion of gaps in the Kenyan health system provided fertile ground to develop action points on maternal healthcare that participants then presented on the second day of the meeting to several Kenyan members of parliament. Ideally, this will be the first discussion of many as maternal health advocates, field workers, and researchers coalesce around ways to address the gaps in maternal healthcare in Nairobi and elsewhere.
Emily Puckart is a senior program assistant at the Maternal Health Task Force (MHTF).
Photo Credit: Jonathan Odhong, African Population and Health Research Center.