-
‘Marketplace’ and ‘NewsHour’ Highlight Population, Health, and Environment Program in the Philippines
›The Danajon reef is the only double barrier reef in the Philippines, “one of the richest marine biodiversity hot spots in the world,” and it’s being devastated as the country’s exploding population depends on its waters for their food and livelihoods, reported Sam Eaton in a recent two-part series on population, health, and environment issues in the Philippines broadcast last month for American Public Media’s Marketplace and the PBS NewsHour.
The report is part of joint project called Food for 9 Billion, with Homelands Productions, the Center for Investigative Reporting, APM, and PBS. Previous reports examined food security in East Africa and Egypt.
The Philippines “import more rice than any other country on the planet,” said Eaton. The “highest population growth rates in all of Southeast Asia” as well as dwindling natural resources – nearly 100 million people live in a land area the size of Arizona – have created a cycle of poverty. The first step to breaking that cycle, he said, is improving access to family planning.
Growing Families, Growing Poverty
The Canayong family, living on the edge of a garbage dump in a Manila slum, offers a vivid example of what poverty means in the Philippines. Clarissa Canayong has had 14 children – 4 died from measles and dengue fever, the remaining 10 spend their days alongside Clarissa, sifting through the dump for things they need and things they can sell. At the end of a good day, the family has earned around $7 to survive on. All in all, Clarissa’s “inability to provide enough food, and to pay for her children’s education, all but guarantees she and her family will remain poor,” said Eaton.
The archipelago adds about two million people every year, putting population on track to double in size sometime around 2080. “And that’s only if something is done to close the birth control gap,” said Eaton, as those projections build in an expectation that growth will slow.
“As cities all across the country expand, the displaced often end up migrating to urban slums,” he said. “Population growth among poor Filipinos is twice the national average,” meaning that once a family enters poverty, they end up in a cycle “that’s nearly impossible to break.”
The Difference Family Planning Can Make
If Clarissa had had access to family planning, she told Eaton, she would have wanted to have only two children. In Humayhumay, where residents have access to a community-based family planning distribution program started by PATH Foundation Philippines, Inc., families have that luxury of choice.
Working through local partners, the PATH Foundation identifies and trains community-based vendors to sell contraception – both pills and condoms, said Dr. Joan Castro, who began the program in Humayhumay. The idea is to make buying contraceptives “as easy as buying soft drinks or matches.”
Both Jason Bostero, a farmer and fisherman in Humayhuay, and his wife, Crisna, grew up in large families – so large, in Crisna’s case, that “sometimes, we would only eat once a day because we were so poor. We couldn’t go to school. I did not finish school because there were just so many of us,” she told Eaton.
Now that they have access to contraceptives, a smaller family size means their income is “just right” to feed everyone three times a day. For the community as a whole, smaller family sizes mean that the nearby fish stocks that provide the community with food and income have a chance to replenish themselves in the absence of overfishing.
“In just six years since the program was first established here,” reported Eaton, “family sizes have plummeted from as many as 12 children to a maximum of about 4 today.”
Exception to the Rule
Humayhumay is an exception to the rule in the Philippines. There is no state funding for birth control in the country, and over the past few years, major international donors like USAID and the United Nations have ended their family planning work in the country. More than a quarter of poor Filipinos have no access to any type of family planning service, and more than half of all pregnancies are unintended, said Eaton.
Family planning has long been a contentious issue in the country. Eaton spoke to Congressman Walden Bello, who has spent more than a decade trying to pass legislation to establish universal access to birth control and improve other family planning and reproductive services. The Catholic Church, said Bello, is a powerful (80 percent of Filipinos are Catholic) and consistent opponent. In October 2010, the Church went so far as to threaten President Benigno Aquino with excommunication after he voiced support for access to contraception.
Rather than limit population growth, the Church argues the country should increase food production. But land is limited, rice imports are already the highest in the world, and, “according to the World Bank, every major species of fish here shows signs of severe overfishing,” said Eaton.
Looking Forward and Abroad
Eaton pointed to the Philippines’ neighbors as examples to emulate: “A long history of government-supported family planning has…paved the way for Thailand to become one of the world’s biggest rice exporters” and helped to cut back poverty in the country, said Eaton.
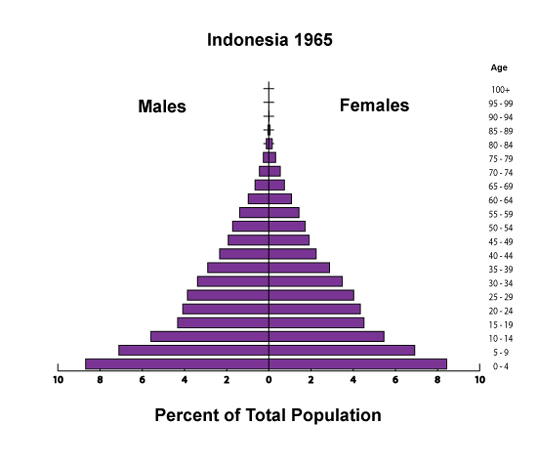
Indonesia too, he pointed out, has largely avoided the population growth-resource depletion-poverty cycle, thanks in part to a state- and faith-backed family planning program. (As Elizabeth Leahy Madsen wrote in a recent New Security Beat post, the decision of Indonesia’s religious leaders to throw their support behind family planning in the 1960s was a key factor in success there.)
Considering the obstacles, the Philippines face an uphill battle before family planning services become similarly universal. But the political tides may already be turning: last April, the President said he would support the reproductive health legislation even if it meant excommunication.
Meanwhile, PATH Foundation’s Castro is hopeful that Humayhumay’s success story will lay the seeds for widespread public support for family planning. “The vision of the project is in this community you see more children educated who are able to become leaders and speak out for themselves in the future and be able to become stewards of their own sexuality and the future environment,” said Castro. “This is the legacy.”
Sources: BBC, Bloomberg News, Catholic News Agency, The Guardian, Population Reference Bureau, TIME Magazine, US Agency for International Development, U.S. Catholic. -
Eric Zuehlke, Population Reference Bureau
Democratic Republic of Congo and Madagascar Connect Family Planning With Environmental Health
›February 10, 2012 // By Wilson Center StaffRemote rural communities in developing countries typically face the related challenges of extreme poverty, poor health, and environmental degradation. And population growth often exacerbates these challenges. In communities that face environmental challenges along with high fertility and high maternal and child mortality, health programs that include family planning can have great benefits for the health and well-being of women and families, with positive influences on the local environment. Meeting the reproductive health needs of women and ensuring environmental sustainability by connecting family planning with environment programs has proven to be a “win-win” strategy. Yet this connection has often been seen as controversial or irrelevant to environmental policymaking.
-
Political Demography: How Population Changes Are Reshaping International Security and National Politics (Book Launch)
›
“The world’s population is changing in ways that are historically unprecedented,” said Jack Goldstone, George Mason University professor and co-editor of the new book, Political Demography: How Population Changes Are Reshaping International Security and National Politics. [Video Below]
-
P.H. Liotta, Salve Regina University
The Real Population Bomb: Megacities, Global Security, and the Map of the Future (Book Preview)
›February 8, 2012 // By Wilson Center Staff There was a time when the city was the dominant political identity. Centuries and even millennia ago, the most advanced societies in the Mediterranean, the Near East, and South America revolved around cities that were either states in themselves or were the locus of power for larger empires and kingdoms. The time of the city is coming again, though now in a considerably less benign way.
There was a time when the city was the dominant political identity. Centuries and even millennia ago, the most advanced societies in the Mediterranean, the Near East, and South America revolved around cities that were either states in themselves or were the locus of power for larger empires and kingdoms. The time of the city is coming again, though now in a considerably less benign way. From the introduction to The Real Population Bomb:
From the introduction to The Real Population Bomb:There was a time when the city was the dominant political identity. Centuries and even millennia ago, the most advanced societies in the Mediterranean, the Near East, and South America revolved around cities that were either states in themselves or were the locus of power for larger empires and kingdoms. The time of the city is coming again, though now in a considerably less benign way.
This book is about where and how geopolitics will play out in the twenty-first century. Cumulatively it represents two decades of work from authors with seemingly dissimilar backgrounds: one is a poet, novelist, and translator; the other is a security analyst and expert in disaster response and management who has worked for two presidential administrations. Both were colleagues at the U.S. Naval War College in the early 2000s.
With the rise of massive urban centers in Africa and Asia, cities that will matter most in the twenty-first century are located in less-developed, struggling states. A number of these huge megalopolises – whether Lagos or Karachi, Dhaka or Kinshasa – reside in states often unable or simply unwilling to manage the challenges that their vast and growing urban populations pose. There are no signs that their governments will prove more capable in the future. These swarming, massive urban monsters will only continue to grow and should be of great concern to the rest of the world.
We have traveled widely and conducted fieldwork in places as disparate as the Altiplano of Bolivia; Caracas, Venezuela; Guayaquil, Ecuador; the autonomous Altai Republic in deep Siberia; and the massive slums of Egypt, India, Kenya, South Africa, and Brazil. What we share from this experience is the recognition that the world has changed before our eyes. Terms such as the “developed” and “developing” world – phrases that were always dangerous and loaded with false value – no longer have the relevance they seem to have had once. Concepts such as “first world” and “third world” are stubborn relics of Cold War thinking – just as our “mental maps” are grounded in the often difficult but known past. We must change our ways of seeing the world.
Traditionally there have been two general approaches to understanding societies and states. One is the humanitarian or ecological perspective in which the focus is on society – how people live and are affected by war, pollution, and economic globalization. The other is a realist perspective in which the focus is on the economic, political, and military relations among major powers such as the European Union, the United States, China, and Russia.
What these traditional approaches underemphasize is the overlap and natural alignment between them. To understand the map of the future, we need to critically appreciate how astonishing population growth in cities – particularly fast-growing megalopolises in weak or failing states in Africa, the Middle East, and Asia – is impacting ecology and ecosystems, human security, and the national security of Western states, as well as allies and trading partners.
For both better and worse, globalization and urban population growth have changed political and economic dynamics in ways that previous conceptions of how the world works cannot do justice. In this book we examine how developments below the nation-state level – at the municipal level – affect how we must see the world of the future. While this work is anything but a travelogue, we do visit some of the most alarming locations on the earth. Often these places have been viewed in impressionistic terms, as distant locations where “others” live – with whom “we” have little interaction. But we are far more connected than we think; whether Nigeria or Pakistan, Bangladesh or Egypt, their future is also ours. The odds seem stacked against those who live there. In the dense, overgrown neighborhoods and shantytowns of Lagos, Kinshasa, Cairo, Karachi, Lahore, or Dhaka, government authorities have failed to provide infrastructure and public services. We need urgent, collective, and innovative actions to help critical megacities weather the gathering storm.
But there is hope and strength. Though time is running short, solutions are still possible. In the end, this book is about the power and resilience of the human spirit.
P. H. Liotta’s latest book is The Real Population Bomb: Megacities, Global Security, and the Map of the Future, with James F. Miskel. As a member of the United Nations Intergovernmental Panel on Climate Change UN’s IPCC, he shared the 2007 Nobel Peace Prize.
Photo Credit: “Urban View: the Republic of Korea’s Second Largest City,” courtesy of United Nations Photo. -
Water and Population: Limits to Growth?
›February 3, 2012 // By Laurie Mazur
Water – essential, finite, and increasingly scarce – has been dubbed “the new oil.” Experts debate whether human societies are approaching “peak water,” beyond which lies a bleak future of diminishing supplies and soaring demand. Others observe that, for many, the water crisis has already arrived.
-
What Would It Take To Help People ‘and’ the Planet?
›February 1, 2012 // By Geoffrey D. DabelkoThe original version of this article first appeared in the “Scientist’s Soapbox” column of Momentum magazine’s special issue on “what would it take” to craft solutions to some of the Earth’s toughest challenges.
People living in the most biodiverse areas of the world tend to be poor, isolated, and dependent on natural resources. They often lack reliable access to alternative livelihoods and health services and thus can place stress on these ecologically unique regions.
Conservation efforts will merely slow habitat loss if they don’t fundamentally address the living conditions of the human residents as well as the flora and fauna. But programs to assist these communities have commonly focused on one problem at a time, reflecting the interests of the funders: Environmental groups focus on conservation, while health organizations concentrate on disease. We must ask whether investments to protect biologically rich areas are effective and sustainable if they don’t respond to the many needs of the people who live there.
But the problems faced by people in these remote areas don’t fit our traditional sectors. The way we disburse our funds, divide our bureaucracies, demarcate our disciplines, and measure success ignores the reality of intersecting needs. Such stovepiping can disrespect the communities’ scarce resources, especially their time. It can waste development aid on duplicate supplies and staff. And it can lead us to miss how the solution to one problem (e.g., providing antiretroviral drugs to treat HIV/AIDS) can be undercut by another (e.g., lacking access to safe water with which to take the pills).
So, what would it take to help particularly vulnerable populations while protecting particularly important ecological systems?
We need to strategically target our help by addressing HELP – health, environment, livelihoods, and population – through a truly integrated approach to sustainable development in these areas. Evidence suggests tackling problems concurrently can be more efficient and effective. Key donors such as the U.S. Agency for International Development are increasingly prioritizing integrated responses, providing some funding for sustainable development innovators and supporting evaluation of the results. But we need more evidence that these efforts can achieve results that match or exceed the outcomes of single-sector projects. To rigorously test this approach, more projects must be funded, implemented and analyzed, over longer periods of time and at bigger scales.
To date, some promising projects and research in diverse locations – Ethiopia, Nepal, Madagascar, Rwanda, the Philippines, and Uganda – suggest that the HELP approach offers greater benefits than traditional programs.
In the Philippines, for example, the PATH Foundation Philippines’ Integrated Population and Coastal Resource Management (IPOPCORM) program addresses pressing needs for both family planning services and sustainable environmental stewardship in densely populated coastal communities, where local fisheries have been depleted because of increased demand for food. IPOPCORM helps create marine protected areas and promotes alternative economic livelihoods such as seaweed harvesting, thus allowing critical local fish stocks to recover. Concurrently, the initiative mitigates human-induced pressures on the environment and lowers the vulnerability of this underserved population by providing voluntary family planning services. Since its launch in 2001, the IPOPCORM program’s approach has yielded measurable benefits, simultaneously reducing program costs and improving health and environmental outcomes – and outperforming compartmentalized, side-by-side sector interventions.
How can we bring HELP to biodiversity-rich communities? First, we can encourage scholars, practitioners, and policy-makers to step outside their stovepipes by producing and distributing manuals, for example, based on lessons learned from existing cross-disciplinary projects. Second, we must bridge the gap between analysis and field-based programs by developing new metrics that better assess the impact of integrated programs. Third, we must open up bureaucratic funding structures by demonstrating not only the short-term savings but also the synergies that bolster long-term sustainability.
The challenges are significant, but I see promising new opportunities for overcoming them. For example, the new Pathfinder International-led projects around Lake Victoria in Uganda and Kenya mark the entry of a respected health organization into the environmental arena and the return of a leading private funder – the MacArthur Foundation – to HELP programs. With some of Africa’s highest population densities, poverty, ethnic diversity, and biodiversity, the Great Lakes region is one of the most volatile intersections of human development and environmental change.
Through these and other community-based, integrated projects, we can truly help people and the planet at the same time.
Photo Credit: “Boy on road east of Addis,” courtesy of Geoff Dabelko/Wilson Center. -
Indonesia: Pioneering Community Outreach Creates Success Story
›January 31, 2012 // By Elizabeth Leahy MadsenThis is the third post in a series profiling the process of building political commitment in countries whose governments have made strong investments in family planning. Previous posts have profiled Rwanda and Iran.
While the two other countries profiled in this series, Rwanda and Iran, have only reinvigorated their family planning programs within the past 20 years, Indonesia’s story begins in the 1960s. In this respect, the world’s fourth most populous country is classified among the pioneers of family planning in the developing world and has been described as a “world leader” and “one of the developing world’s best.” An extensive community outreach program combined with a centralized government that made family planning a priority were key to Indonesia’s success story.
Jakarta Pilot and Religious Support Motivates National Scale-up
For a decade and a half after the struggle for independence from the Dutch ended in 1949, the government of President Sukarno ruled out any government support for family planning. According to a Demographic and Health Survey (DHS) report, the rate of contraceptive use among married women at the time was essentially zero. Fertility rose slightly during this period, from an average of 5.5 in the early 1950s to 5.6 children per woman a decade later. However, in 1965, Sukarno was overthrown, and the next year, a military general named Suharto assumed power in an uprising that left as many as half a million people dead.
Suharto’s regime would last until 1998. Though he operated with a “heavy hand” amidst personal corruption, Suharto also aggressively pursued economic development and brought about a policy shift towards promoting family planning. Despite initial reservations – Suharto believed that the people would oppose family planning on religious grounds – various domestic and international advisers convinced him otherwise.
General Ali Sadikin, the governor of Jakarta – a city of three million even then – was particularly influential in convincing Suharto. According to Australian demographer Terence H. Hull, who has written extensively about population issues in Indonesia, Sadikin was “quickly learning demographic lessons in his attempts to renovate a city with poor housing, schooling, transport, and basic services,” and he began to regularly speak out about the challenges that rapid population growth posed to his goals of urban development.
Sadikin decided to support the Indonesian Planned Parenthood Association, which had a network of clinics offering family planning, but lacked the funding to meet more than a small amount of demand. With the public support of Sadikin, a Jakarta-wide pilot program was operational in 1967.
Hull reports that a second integral event in the early years was a 1967 meeting between government officials and Muslim, Protestant, Catholic, and Hindu leaders representing four of the country’s major religions. Following the meeting, a pamphlet called “Views of Religions on Family Planning” was published, representing “a tipping point when national consensus around the morality of birth control was turning from strongly negative to strongly positive.”
A Strong Coordinating Board Reaches out to Communities
By late 1968, efforts were in place to scale up the family planning program in Jakarta to the national level. The National Family Planning Coordinating Board (BKKBN in Indonesian) was created and quickly became entrenched throughout the country thanks to generous funding, including from international donors.
The BKKBN’s emphasis on the community level, which ensured that family planning services and awareness-generating activities were reaching people around the country through multiple channels, was a key factor in the program’s achievements. The organizations involved in promoting family planning messages at the community level included youth, women’s and religious groups, employers, and schools, with high-level support reiterated regularly by the president. Hull described the BKKBN’s efforts as “a true collaboration because the program emphasized institutions not normally associated with family planning, but did so in a way that was both socially acceptable and socially invigorating.”
In the program’s first two decades, the contraceptive prevalence rate for modern methods rose from almost nonexistent to 44 percent, and fertility subsequently fell from 5.5 to 3.3 children per woman. These changes are widely attributed to robust government sponsorship from the highest levels, together with effective grassroots implementation that fostered support from nearly all sectors of society.
In subsequent years, Indonesia experienced rapid economic and social development. Per capita income increased more than 20 times over between 1966 and 1996, with initial growth largely due to oil revenues. Other development indicators also improved dramatically. The literacy rate is now over 90 percent, nearly all girls attend school, and half of women are members of the labor force. However, Hull cautions against proclaiming the family planning program the primary causal factor in these successes. Family planning and other development programs would not have been as effective, he says, without changes in the political structure, which steadily became more centralized and stable in its oversight of a very heterogeneous society.
A Recent Plateau
As Indonesia continued to develop and its political system evolved, the family planning program has faced some challenges in the past 15 years. Suharto resigned in the face of widespread opposition in 1998, after more than 30 years in power. While this brought positive movement towards democracy, the ensuring political uncertainty shifted the government’s energies away from reproductive health and other aspects of social development.
In the early 2000s, the family planning program was decentralized to district and municipal levels, in line with political reforms aimed at diminishing the role of central hierarchy nationwide. District leaders were charged with planning, budgeting, and implementing family planning and other primary health services. In accordance, BKKBN modified its strategies to become even more community-oriented. Still, observers judge the family planning program to have “weakened” following decentralization.
With strong logistics, popular support, and donor assistance, contraceptive use continued rising during the years of political transition. By 2002-2003, 57 percent of married women were using a modern contraceptive method and the fertility rate had reached 2.6 children per woman. However, these indicators remained unchanged in the next national survey, conducted in 2007. Fertility in Indonesia is at the median for Southeast Asia – higher than Thailand and Vietnam and lower than Cambodia and the Philippines.
The Program Moves Forward
As democracy became more secure in the early 2000s, the country’s next generation of leaders kept sight of demographic issues. In 2005, President Susilo Bambang Yudhoyono stated, “High population growth without rapid economic growth will result in poverty and setbacks … Large numbers of children and high populations will only bring advantages if they are skilled.” BKKBN and the Ministry of Health worked with USAID, public health researchers, NGOs and others to develop national family planning standards for quality of care, which were devised and implemented in the early 2000s.
Judging the program’s achievements to have been substantial and its momentum sustainable, USAID graduated Indonesia from population assistance in 2006, after 35 years. Though gaps remain, women’s fertility preferences are largely being met.
Today, 80 percent of all births are intended, and unmet need for family planning – the share of married women who wish to delay or prevent pregnancy but are not using contraception – stands at nine percent, two percentage points below the average for Southeast Asia and all developing countries. Meanwhile, Indonesia’s demographic profile looks much different than it might have. At the time of graduation, USAID reported that without its long-standing and well administered family planning program, Indonesia’s 2006 population would have been larger by 80 million people, or 35 percent.
Elizabeth Leahy Madsen is a consultant on political demography for the Wilson Center’s Environmental Change and Security Program and senior technical advisor at Futures Group.
Sources: Demographic and Health Surveys; Hull (2007); Management Sciences for Health; New York Times; UN Population Division; USAID.
Photo Credit: “Jakarta,” courtesy of flickr user frostnova. -
‘New Security Beat’ Is Five Years Old
›January 26, 2012 // By Wilson Center Staff
ECSP’s Sean Peoples, Meaghan Parker, and Schuyler Null accepted the Population Institute’s Global Media Award for Best Online Commentary at a January 12 ceremony in New York City. Five years ago, in January 2007, we launched New Security Beat. Since then we’ve established a strong editorial focus on a key but neglected niche: where population, environment, and security meet.
Showing posts from category global health.